Dr. Paresh Bang | Matruchhaya Spine Clinic
Meet Our Doctor
Dr. Paresh Bang
Consultant Spine Surgeon

Spine Fusion Surgery In Jabalpur
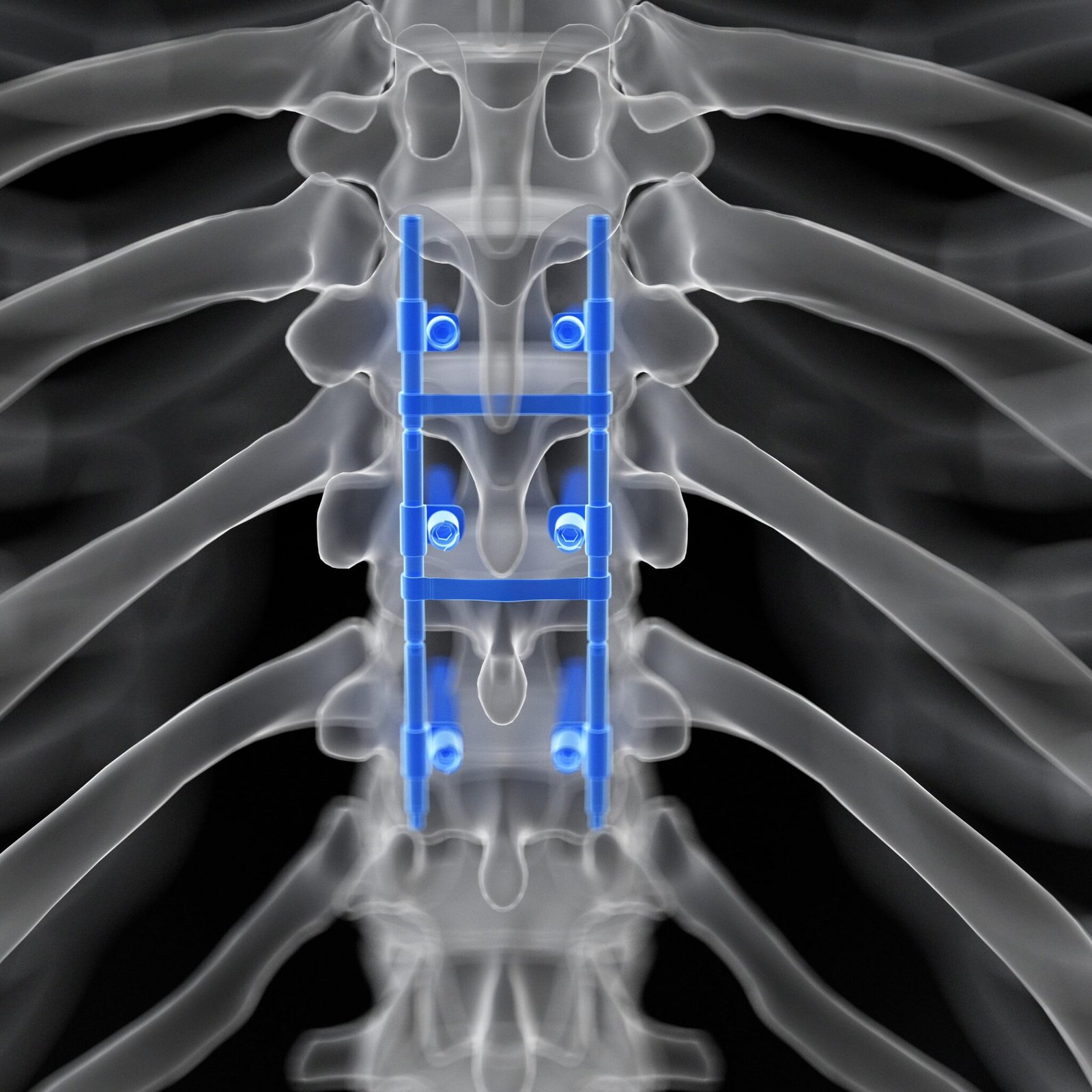
some cases, spinal fusion might be considered the best option for a patient.
What does spinal fusion treat:
- A spinal fusion can address pain, numbness, muscle weakness and much more. Weakness anywhere along your spine can cause pressure on your spinal cord or the nerves branching off of it. Pressure on our spinal cord or nerves can interfere with signals traveling through them. Spinal fusion treats conditions can affect our vertebrae or the joints of soft tissue that support and connect your vertebrae.
The conditions that illustrate this are such as include: - Congenital spine conditions. This is when you are born with these conditions.
- Herniated or bulging, slipped, or ruptured disks.
- Bone or soft tissue infections of your spine.
- Pinched nerves in your neck or lower back and cause of sciatica due to cervical radiculopathy.
- Scoliosis as it occurs in both adults and children.
- Spondylolisthesis.
- Spondylosis.
- Spinal stenosis, foraminal stenosis.
- Fractures and injuries to the spine.
- Tumors of bones, soft tissues, or nervous tissue such as the spinal cord or nerves in and around your spine.
How the Procedure Works:
Some of the most likely of those include:
- A medical check-up and laboratory tests before surgery :our surgeon would want to be assured that you are healthy before this procedure. our surgeon will test you in order to look for problems you can’t feel or that may not cause symptoms, such as high blood pressure, clotting problems, and your kidney functions.
- Medication review: Be sure to make all of the surgical staff aware of everything you take, not just the medications given by your doctor, but any vitamins, supplements or other things you take for your health, so when you are in surgery they can give appropriate attention to medications and their potential affect on your surgery. Similarly, be sure to follow your provider’s instructions about prescriptions exactly as given. That can make difference to the safety of our surgery and recovery.
- Support planning: You will have restrictions for some time after your surgery—such as lifting and driving—that can be very difficult to manage independently. You should be confident of someone’s ability to help you at home until the restrictions are lifted.
- Anesthesia planning: You will meet with an anesthesiology team before your surgery. They will review anesthetic choices that might be available during your surgery, and make recommendations about which to use.
- Blood supply planning: Most people won’t ever require a blood transfusion during spinal fusion surgery, but your doctor may want to discuss your options beforehand as a precaution.
- Nicotine use review and recommendations: Nicotine use — including smoking, vaping or tobacco — can seriously disrupt body’s ability to heal and rebuild bone tissue after (which is vital to this surgery being as effective as possible).
- Cleansing:You may be provided with instructions and supplies to cleanse the day of or the day before your procedure.
- Eating and drinking: Your provider will also provide you with instructions on stopping food and liquids (fasting) before your surgery.
Types of Spinal Fusion:
The specific type of spinal fusion surgery depends on location of problem in spine and the approach used by the surgeon. There are several common methods:
- Posterior Lumbar Interbody Fusion (PLIF): In this technique, the surgeon approaches the spine from the back (posterior) and removes the damaged disc. A bone graft or cage filled with bone is then inserted between the vertebrae, and screws and rods are used to stabilize the spine.
- Anterior Lumbar Interbody Fusion (ALIF): spine is approached from the front (anterior), and damaged disc is replaced with a bone graft or a spacer. This method avoids cutting through large back muscles and is typically used for lumbar fusion.
- Transforaminal Lumbar Interbody Fusion (TLIF): The surgeon approaches the spine from the side and back, which can provide a more direct path to the vertebrae while minimizing disruption to muscles and nerves.
- Lateral Interbody Fusion (XLIF): This is a minimally invasive approach where the spine is accessed from the side of the body. It is used primarily for lumbar spine fusion.
- Cervical Fusion: Performed in the neck region (cervical spine), this surgery is usually done via an anterior approach (from the front of the neck) or posterior approach (from the back). It is often used to treat cervical spondylotic myelopathy, herniated discs, or fractures.
What happens during the spinal fusion:
The various types of spinal fusion surgeries will depend on the portion of your spine that needs to be reached, as well as what kind of fusion is required. Some of these variables include:
- The direction of approach: Approaches are made to your spine from your back, front, side, or combination of each.
- Type of incision: Some spinal fusions are better done by open surgery while others may be much better suited to a minimally invasive operation. Each has its advantages, and your surgeon will have spoken to you about which is best for you and your particular spine problem.
- Materials used: Bone tissue (with hardware) is most commonly used in a spinal fusion to add strength or reinforcement to the fusion. Your body will perceive the bone tissue as part of the healing process and accelerates that process. The bone tissue can be autologous, coming from elsewhere in your body, or it can come from a cadaver donor, or it can be artificial bone-like material, synthetic. Your surgeon will further support the fusion of the vertebrae by incorporating hardware, such as screws, plates, or rods. Be sure to discuss any metal allergy you have with your healthcare provider.
- Other procedures or steps. You might need additional related procedures or steps to the surgery that addresses any issues that might be causing or contributing to your spine issues. Many of these are forms of spinal decompression surgery.
All of the portions of the spinal fusion being complete, your surgeon will close up the incision(s) using surgical staples, sutures or some other means. Some of these sutures must be taken out, while others your body absorbs on its own. Your provider will let you know what kind you have, and if you’ll need to come in for a visit to have them removed.
After the operation, your care team will bring you into a recovery space in which:
A team helps you out of anesthesia, manages your surgical pain, and then establishes safety enough to return you to your hospital room.
You can see your loved ones, although you probably will have very little memory of this.
You might wake up and see that there are several different tubes that have been placed inside. There may be a catheter in your bladder, and lines placed in your veins, probably feeding you fluids and other medications.
How long does spinal fusion surgery take:
Your time in the operating room is comprised of many more steps than the time involved in the actual surgery. Spinal fusion can take up to five hours. The time involved in the surgery will depend on what you need and your situation, so no one but your provider will be able to give you an accurate estimate of how long your surgery might be.
What happens after spinal fusion surgery:
The type of surgery may also determine the next procedure-whether it is an inpatient or outpatient type. Your surgery most likely was an outpatient procedure if you went home the same day or the following morning after your surgery. Otherwise, surgery usually requires an inpatient procedure; you probably had to spend a couple of days in the hospital.
Depending on the kind of surgery that you have undergone or to which you have a medical case, you might need to learn how to hold yourself and maintain posture. That can affect how we sit, stand, walk, and move. may also need to use some kind of brace or support.
While you are in recovery, your provider will instruct you to avoid certain activities and types of movements for some period of time. This means that you will need to be assisted with many tasks, some of which may seem really simple. It’s important that you follow your provider’s guidance regarding activity limitations. Better safe than sorry when you do something that upsets your recovery.
Your doctor might also recommend you to get some post-surgery physical therapy. Generally, this will be several weeks after your surgery. Physical therapy helps you get back to strength and healing yourself from the surgery. It can also help you with adjusting to altered motion of your back as a result of the surgery.
Recovery Process:
- Hospital Stay: Typically, patients spend 2-4 days in the hospital, though this can vary depending on the complexity of the surgery.
- Pain Management: Medications are used to the manage pain after surgery.
- Physical Therapy: Rehabilitation is crucial for the successful recovery. Physical therapy helps to strengthen the muscles supporting the spine and improve mobility.
- Fusion Process: It can take several months to a year for the vertebrae to fully fuse. During this time, patients need to a avoid strenuous activities.
Risks and Complications:
Like any major surgery, spinal fusion comes with risks, including:
- Infection: As with any surgery, there’s the risk of infection.
- Bleeding: Excessive bleeding during and after the surgery.
- Nerve Injury: Nerves surrounding the surgical area may be damaged, causing numbness or weakness.
- Non-union: Sometimes the bone does not fuse properly, which might require additional surgery.
- Adjacent Segment Disease: Stress on adjacent vertebrae, which can lead to degeneration in nearby areas over time.
Benefits:
- Pain Relief: The primary goal of spinal fusion is to relieve chronic back and neck pain.
- Stabilization: It provides stability to a spine that is unstable due to conditions such as spondylolisthesis or fractures.
- Correction of Deformities: It can be used to correct spinal deformities like scoliosis.
Alternative Treatments:
Spinal fusion is typically recommended only when other treatments have failed. These alternatives might include:
- Physical therapy
- Anti-inflammatory medications
- Spinal injections
- Chiropractic care
How Spinal Fusion Works:
- Bone Grafting: The surgeon places a bone graft between the vertebrae that need to be fused. This graft may be from a patient’s own body (autograft) and a donor (allograft). Artificial graft materials are also used.
- Hardware: Screws, rods, or plates may be used to hold the vertebrae together while the bone heals and fuses the vertebrae over time.
- Recovery: Spinal fusion can take several months for the bones to a fully fuse. Physical therapy is often part of recovery to regain strength and flexibility.Contact Us
Why Spinal Fusion Surgery is Performed:
Spinal fusion is often recommended for a following conditions:
- Degenerative Disc Disease: When discs that act as cushions between vertebrae deteriorate, leading to pain and instability.
- Spinal Stenosis: A narrowing of the spinal canal that can compress nerves, causing pain, numbness, or weakness.
- Scoliosis and Kyphosis: Abnormal curvatures of a spine.
- Spondylolisthesis: A condition where one vertebra slips forward over the one below it, leading to pain and instability.
- Fractures: Vertebral fractures from trauma or osteoporosis that cause instability.
- Infections or Tumors: Infections or tumors that affect the spine and cause instability.Visit Our Hospital
